- Doctors & Departments
-
Conditions & Advice
- Overview
- Conditions and Symptoms
- Symptom Checker
- Parent Resources
- The Connection Journey
- Calm A Crying Baby
- Sports Articles
- Dosage Tables
- Baby Guide
-
Your Visit
- Overview
- Prepare for Your Visit
- Your Overnight Stay
- Send a Cheer Card
- Family and Patient Resources
- Patient Cost Estimate
- Insurance and Financial Resources
- Online Bill Pay
- Medical Records
- Policies and Procedures
- We Ask Because We Care
Click to find the locations nearest youFind locations by region
See all locations -
Community
- Overview
- Addressing the Youth Mental Health Crisis
- Calendar of Events
- Child Health Advocacy
- Community Health
- Community Partners
- Corporate Relations
- Global Health
- Patient Advocacy
- Patient Stories
- Pediatric Affiliations
- Support Children’s Colorado
- Specialty Outreach Clinics
Your Support Matters
Upcoming Events
Colorado Hospitals Substance Exposed Newborn Quality Improvement Collaborative CHoSEN Conference (Hybrid)
Monday, April 29, 2024The CHoSEN Collaborative is an effort to increase consistency in...
-
Research & Innovation
- Overview
- Pediatric Clinical Trials
- Q: Pediatric Health Advances
- Discoveries and Milestones
- Training and Internships
- Academic Affiliation
- Investigator Resources
- Funding Opportunities
- Center For Innovation
- Support Our Research
- Research Areas

It starts with a Q:
For the latest cutting-edge research, innovative collaborations and remarkable discoveries in child health, read stories from across all our areas of study in Q: Advances and Answers in Pediatric Health.


Ava: CDH Diagnosis After Birth

Cassie Holt's labor for her second daughter was so uneventful she took a nap. The doctor woke her up and told her it was time to have a baby. Forty-five minutes later, Ava Holt was born.
She didn't draw a first breath.
"The nurses suctioned her," Cassie recalls. "They thought she had gunk in her lungs."
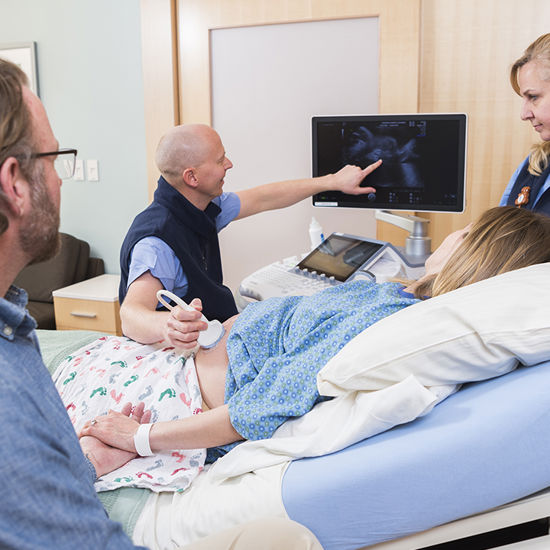
A chest X-ray revealed a far worse diagnosis: Ava had congenital diaphragmatic hernia (CDH). Essentially a hole in the diaphragm, CDH is usually diagnosed in utero, at the 16-week ultrasound. That allows providers to develop a birth plan and, often, to surgically intervene before birth using a fetal surgery known as fetoscopic endoluminal tracheal occlusion (FETO). But Ava's case had been subtle.
The opening had allowed Ava's abdominal organs to drift into her chest, crowding her lungs. The result was pulmonary hypoplasia: Her stunted lungs couldn't supply her body with enough oxygen to survive.
CDH outcomes among the best in the country
A ventilator wouldn't be enough. Ava needed a team with the equipment, expertise and experience to keep her alive. Children's Hospital Colorado's flight team airlifted Ava and her father from their home in Casper, Wyo., to the Colorado Fetal Care Center in Aurora, Colo. There, pediatric surgeon Kenneth Liechty, MD, and a dedicated CDH team were waiting for her.
She was in good hands.
"Our CDH outcomes are among the best in the country," says Dr. Liechty. "We have the meds, the treatment plans, the 24/7 surgical team to repair the diaphragm, the neonatal team to support recovery."
One of those meds, nitric oxide, used to relax the blood vessels of the lungs to maximize blood flow, was pioneered at Children's Colorado. It's now a treatment standard. The neonatal team that first implemented it remains among the top five in the nation. Within hours, Ava stabilized.
"I drove down there the next day, by myself," says Cassie. "I guess that mama bear thing kicked in."
Growing and thriving after CDH
The next day, Dr. Liechty performed surgery to repair her diaphragm and move her internal organs back into place. The configuration is slightly different — Ava's bowels zig-zag up and down instead of wrap in a circle — but it works. "Some centers will use a piece of plastic to repair the diaphragm," says Dr. Liechty. "Here, we use an actual flap of muscle, which will grow as the baby grows."
The operation went smoothly. Ava spent five weeks in Children's Colorado's Level IV NICU — among the most advanced and capable units like it in the nation — while her lungs grew.
Cassie didn't waste that time. She researched. She asked questions. She learned everything she could about Ava's condition and outlook, and she talked to other parents she met in the NICU with babies in the same boat. Some she still keeps up with today.
Ava is 3 years old now, and while she's been late on a few milestones — she took her first steps at 18 months — she's otherwise indistinguishable from any 3-year-old.
"Just this morning, we went on a 3-mile hike." Cassie laughs. "I mean, we didn't really set out to walk that far, but yeah, she's doing great."
Would you like a second opinion?
If you have received a prenatal diagnosis, are considering treatment options or just want to feel more confident about your treatment plan, our fetal care experts are here to help.
Request a second opinion from our Colorado Fetal Care Center



 720-777-0123
720-777-0123



